Healthcare outsourcing has shifted from simple administrative back-office processing to critical, patient-facing clinical support. By integrating Agentic AI and high-touch human expertise, health systems now outsource complex tasks like real-time clinical documentation, prior authorization, and chronic care management to reduce denial rates, improve patient throughput, and sustain fiscal health under value-based care models.
Executive Summary
- The Paradigm Shift: Outsourcing is no longer about labor arbitrage; it is now a strategic partnership leveraging Agentic AI to manage “clinical-adjacent” workflows.
- Denial Management: AI-driven BPO partners can predict denial patterns before submission, potentially reducing claim rejection rates from the industry average of 15% to sub-4%.
- Patient Throughput: Outsourcing telehealth triage and scheduling support increases outpatient throughput by up to 30%, as internal staff focus exclusively on high-acuity care.
- Clinical Efficacy: Ambient listening and AI-scribe integration through BPO partnerships increase direct physician-patient interaction time by over 20%.
- Regulatory Readiness: The 2026 HIPAA Security Rule updates demand rigorous vendor accountability, making “Zero-Trust” outsourcing architectures a mandatory requirement for data compliance.
- Fiscal Impact: Strategic outsourcing models now target a 15-25% improvement in net collection rates by shifting resources from manual data entry to proactive claims appeal management.
The Death of the “Back Office” Narrative
For decades, health systems viewed BPO as a cost-containment lever. CFOs sought lower wages for medical coding or claims processing, treating the BPO provider as a distant utility. This model relied on volume and speed, often ignoring the friction it introduced into the patient journey. Today, that narrative has collapsed.
The pressure of value-based care and tightening margins forces health systems to stop viewing BPO as an administrative expense and start viewing it as a component of their clinical infrastructure. Modern BPO providers now function as the nervous system of a hospital’s digital strategy. They manage the data flows, the patient engagement touchpoints, and the pre-visit clinical documentation that allow providers to practice medicine rather than data entry.
Agentic AI: The New Workforce Standard
The industry has moved beyond simple robotic process automation (RPA). We now operate in the era of Agentic AI-autonomous agents capable of planning, sequencing tasks, and adapting to real-time variables.
Unlike traditional software that requires human instruction for every step, an agentic system can identify an incomplete prior authorization request, cross-reference the clinical notes with payer-specific coverage policies, and draft an appeal-all without human prompting. However, raw AI adoption often fails in healthcare due to “hallucination” risks and clinical nuance.
Successful health systems pair these AI agents with a “Human-in-the-Loop” (HITL) architecture. The AI drafts the clinical documentation or insurance appeal, while a medically trained offshore or nearshore professional performs the final sanity check. This combination provides the speed of automation with the risk mitigation of human clinical expertise.
Navigating the 2026 HIPAA Security Rule
The 2026 HIPAA Security Rule updates represent a significant maturation of cybersecurity expectations. The regulatory environment now mandates stricter audit requirements, mandatory multi-factor authentication (MFA), and granular network segmentation.
These rules effectively kill the “do it cheaply and quickly” outsourcing model. Partners must now demonstrate proof of security in real-time. If a BPO partner does not have encryption-at-rest and strict role-based access controls, they are now a massive liability. Hospitals must audit their BPO contracts to ensure they meet these new “Zero-Trust” requirements. Compliance is no longer a checklist; it is an active, ongoing operational process.
Operational Performance Metrics
|
Metric |
Traditional BPO Model |
Next-Gen Strategic Outsourcing |
|
Primary Driver |
Labor Cost Savings |
Operational Efficiency & Outcome Quality |
|
AI Integration |
Basic RPA (Rule-based) |
Agentic AI (Autonomous Agents) |
|
Denial Rate |
10% – 15% |
2% – 4% |
|
Clinical Role |
Administrative Only |
Clinical-Adjacent (Scribing, Triage) |
|
Data Security |
Standard Compliance |
Zero-Trust Architecture |
Bridging the Gap: Clinical-Adjacent Operations
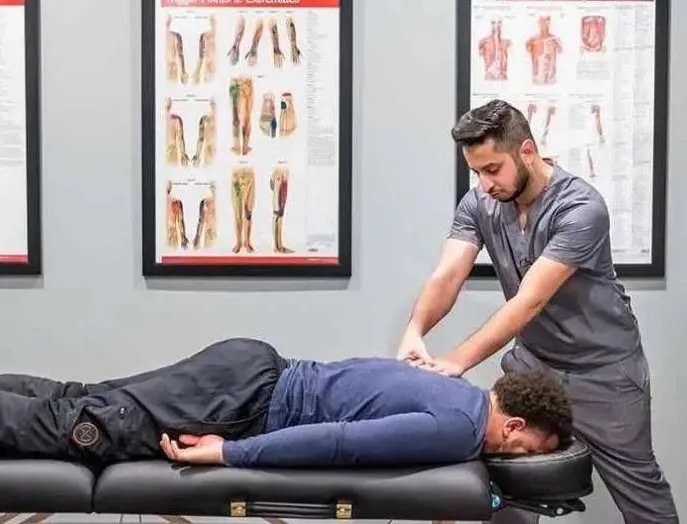
The most transformative change in healthcare BPO is the move into clinical-adjacent work. This includes real-time clinical scribing, remote patient monitoring (RPM) of chronic care populations, and triage support.
When a hospital outsources these functions, they are essentially extending their clinical care team. For example, by offloading RPM data analysis to a BPO team that uses AI to flag anomalies, physicians receive prioritized alerts only when intervention is necessary. This prevents the “alert fatigue” common in internal nursing teams and ensures that high-risk patients receive attention exactly when they need it.
Comparing Outsourcing Strategies
|
Strategic Focus |
Impact on System |
Key KPI |
|
RCM Optimization |
Reduces financial leakage |
Days in A/R |
|
Clinical Scribing |
Improves physician satisfaction |
Patient Encounter Time |
|
Prior Authorization |
Eliminates care delays |
Authorization Turnaround |
|
Patient Access |
Improves front-end experience |
No-Show Rate |
Case Study: Reclaiming Patient Throughput
The Challenge:
A regional multi-specialty healthcare system experienced a 14% denial rate across its outpatient services. Prior authorization requirements had increased by 30% over a three-year period, overwhelming internal utilization management teams. Clinicians were spending an average of two hours per day on documentation and appeals, contributing to burnout and a 12% provider turnover rate.
The Intervention:
The organization adopted a clinical-adjacent outsourcing model, transferring prior authorization and non-complex claims management to a specialized partner supported by Agentic AI. The partner implemented an automated workflow in which AI agents reviewed incoming clinical documentation against payer-specific requirements and pre-populated authorization requests. These outputs were then validated by medically trained professionals prior to submission, ensuring both accuracy and compliance.
The Outcome:
Denial rates declined from 14% to 3.5% within six months. Clinician time spent on administrative tasks decreased by 45%, allowing providers to refocus on patient care. The system expanded its outpatient capacity by 20% without increasing administrative headcount. Provider turnover stabilized at 6% within the first year, reflecting improved working conditions and reduced administrative burden.
Expert FAQs
How do we ensure HIPAA compliance with offshore teams under the 2026 rules?
The 2026 rules require a shift to Zero-Trust architectures. You must verify that your partner utilizes end-to-end encryption, mandatory MFA, and regular independent security audits. Avoid partners who treat compliance as a documentation exercise; instead, demand real-time audit logs and evidence of network segmentation.
Can Agentic AI actually replace human billers?
No. It replaces the labor of data entry and routine status checks. It does not replace the judgment required for complex appeals, contract negotiations, or multi-payer denials. The most effective model is a 70/30 split, where agents handle the heavy lifting of data processing and humans handle the strategic exception management.
Is it possible to maintain quality control when scaling outsourced clinical support?
Quality control depends on embedded analytics. Implement a dashboard that tracks your BPO partner’s output against the same KPIs used for your internal staff. Use AI to perform randomized audits of documentation or calls to ensure clinical accuracy and adherence to care pathways.
What is the biggest risk in moving BPO from the back office to the frontline?
The primary risk is the loss of the “human touch” in patient interaction. When outsourcing patient-facing tasks like scheduling or triage, the BPO staff must be trained to match your health system’s cultural standards, communication style, and empathy protocols. They are not just data processors; they are your brand ambassadors.
How should leadership measure the ROI of “Clinical-Adjacent” outsourcing?
Move beyond cost-per-full-time-equivalent (FTE). Measure the impact on physician throughput, patient retention, and clinical quality metrics. If an outsourced scribe saves a physician one hour of documentation time per day, calculate the revenue potential of that reclaimed hour for patient care. That is the true ROI.